Health and Vitamin D – The Vital Connection
Vitamin D, the Sunshine Vitamin, is vital to human health. It is not only a vitamin but is also a vital hormone. Vitamin D has been recognized vital for bone health for about one hundred years. It is responsible for adequate amounts of calcium and phosphorus in our body. Adequate amounts of calcium and phosphorus are indispensable for the normal development and mineralization of the skeleton.
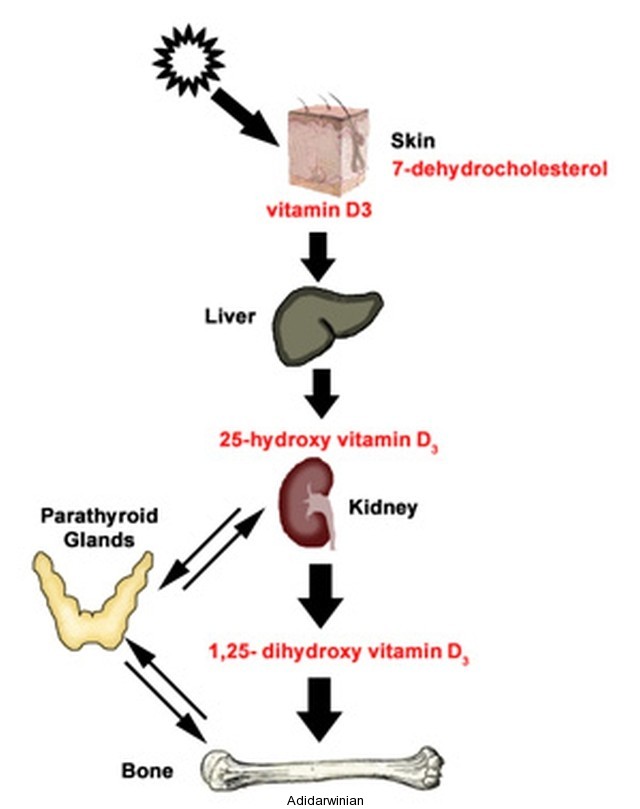
Vitamin D occurs in two forms – Vitamin D3 and Vitamin D2. Vitamin D is the only vitamin which can be made in the skin from exposure to the ultraviolet B radiation of the sunlight. Ultraviolet B radiation, of wavelength 290 nm to 315 nm, penetrates into the human skin and converts a molecule called 7-dehydrocholesterol into Previtamin D3. Previtamin D3 is immediately converted to Vitamin D3. This conversion is a heat-dependent process. When a person excessively exposes to the ultraviolet B radiation of the sunlight, Previtamin D3 and Vitamin D3 degrade into inactive products.
 Vitamin D3 is present in oil rich fishes, such as, Salmon, Tuna Ahi-YT, Trout Farm, Blue fish, Cod, Tuna, Mackerel, Sardines, and Herring. Commercially available Vitamin D3 is synthesized from the precursor of cholesterol (7-dehydrocholesterol). This compound is naturally present in the skin or is obtained from the Lanolin. Lanolin is a yellowish sticky waxy mass of refined wool grease which is secreted by the sebaceous (oil-secreting) glands of wool-bearing animals. It contains about 30 percent incorporated water, and is also called wool wax or hydrous wool fat or wool grease. Vitamin D2 is manufactured through the ultraviolet irradiation of a molecule found in yeast (Ergosterol). Vitamin D2 is found naturally in mushrooms exposed to the sunlight. Both Vitamin D2 and Vitamin D3 are used in Vitamin D supplements.
Vitamin D3 is present in oil rich fishes, such as, Salmon, Tuna Ahi-YT, Trout Farm, Blue fish, Cod, Tuna, Mackerel, Sardines, and Herring. Commercially available Vitamin D3 is synthesized from the precursor of cholesterol (7-dehydrocholesterol). This compound is naturally present in the skin or is obtained from the Lanolin. Lanolin is a yellowish sticky waxy mass of refined wool grease which is secreted by the sebaceous (oil-secreting) glands of wool-bearing animals. It contains about 30 percent incorporated water, and is also called wool wax or hydrous wool fat or wool grease. Vitamin D2 is manufactured through the ultraviolet irradiation of a molecule found in yeast (Ergosterol). Vitamin D2 is found naturally in mushrooms exposed to the sunlight. Both Vitamin D2 and Vitamin D3 are used in Vitamin D supplements.
Vitamin D is a fat soluble vitamin. Vitamin D (Vitamin D represents D3, or D2, or both), after being ingested from the dietary sources, is incorporated into the particles called chylomicrons. Fats, such as triglycerides and cholesterol, are not able to circulate freely in the blood, because human blood is mostly aqueous. To be able to circulate in aqueous human blood, cholesterol and triglycerides are combined with proteins to form lipoproteins. There are different types of lipoproteins, viz. – very low density lipoproteins (or VLDL), low-density lipoproteins (or LDL), high-density lipoproteins (or HDL), and chylomicrons. Chylomicrons are formed from the fats present in food processed by the intestine. Their function is to transport digested fats (as triglycerides) to muscle and fat cells. Chylomicrons get absorbed into the lymphatic system, and then, enter the blood.
Vitamin D that comes from the action of sunlight on the skin or from the dietary sources is biologically inactive and requires undergoing biochemical reactions in the liver and the kidneys. In the liver, Vitamin D undergoes an enzymatic reaction, which is, known as hydroxylation. The result is the conversion of this vitamin into 25 (OH) D. 25 (OH) D is further converted in the kidneys into 1,25 (OH)2 D, also known as Calcitriol. 1,25 (OH)2 D is the biologically active form of Vitamin D. This biologically active form has a crucial role to play in various tissues of our body.
1,25 (OH)2 D stimulates absorption of calcium and phosphorous from our intestine. Without Vitamin D, only 10 % to 15% of dietary calcium gets absorbed. Also, without this vitamin only about 60% of phosphorus gets absorbed. Vitamin D, when present in sufficient amount, enhances absorption of calcium by 30% to 40% and absorption of phosphorus by 80%. Deficiency of this vitamin results in abnormalities in calcium, phosphorus, and bone metabolism. Deficiency causes a decrease in the efficiency of absorption of calcium and phosphorus from diet. This results in the increase in the levels of Parathyroid hormone (PTH), which in turn, leads to mobilization of calcium from the skeleton into blood in order to maintain serum calcium in the normal range. The increase in levels of Parathyroid hormone also increases phosphorus wasting in the kidneys. The PTH also increases activity of osteoclasts (bone cells that dissolve bone), which creates local foci of bone weakness and causes a reduction in bone mineral density (BMD). This results in Osteopenia and Osteoporosis. Osteopenia is a condition in which the bones lose calcium and phosphorous and become less dense. This makes the bones weaker. When bone loss becomes more severe, the condition is known as the Osteoporosis. It is now well established that the deficiency of the Sunshine Vitamin leads to loss of bone matrix and minerals. This loss results in the increased risk of Osteoporosis and fractures. Recent studies have revealed that Vitamin D supplementation decreases the risk of falls. Falls often result in osteoporotic fractures.
Increased loss of phosphorus through the urine, due to increase in the levels of PTH, leads to low serum levels of phosphorus. This results in a calcium-phosphorus imbalance, and causes a mineralization defect in the skeleton. In young children, who have little amounts of mineral in their skeleton, this defect results in a multitude of skeletal deformities known as Rickets. In adults, as there is enough mineral in the skeleton to prevent deformsities in their skeleton, this mineralization defect frequently remains undetected. This mineralization defect in adults is known as Osteomalacia. Osteomalacia causes a decrease in bone mineral density (BMD), and is associated with generalized or isolated pains in the bones and muscles. When Vitamin D deficiency is severe, accumulation of poorly mineralized bone results in Osteomalacia. Osteomalacia is a painful bone disease which is also associated with fractures. Proximal muscle weakness is a major clinical sign of Vitamin D deficiency. Muscle tissue has Vitamin D receptor, and activation of this receptor can promote synthesis of new muscle protein. Studies have found a positive relation between serum 25 (OH) D values and muscular strength and lower extremity function. The efficacy of vitamin D for increasing muscular strength and balance and decreasing the risk of falls has also been shown by some trials.
Other Roles of Vitamin D
The Vitamin D receptors are present in most tissues and cells of our body. The enzyme responsible for the conversion of 25 (OH) D into the biologically active form (1,25 (OH)2 D) is present in a multitude of cells. Most tissues and cells also have the ability to make 1,25 (OH)2 D. Clinical studies have suggested a preventive effect of Vitamin D on a wide range of diseases.
The Sunshine Vitamin, regulates cellular growth and influences the immune system. The studies have provided evidence that this vitamin decreases the risk of cancer. There is compelling evidence that suggests increased risk of common cancers in people living at higher latitudes. It has been suggested that increasing intake of Vitamin D or sun exposure increases the concentrations of Vitamin D 25 (OH), which in turn, is changed to Vitamin D 1,25 (OH)2 in the body tissues – colon, prostate, breast, etc. Vitamin D 1,25 (OH)2 helps in regulating cell growth and reduces the risk for cells to become malignant. Studies have demonstrated an association of Vitamin D deficiency with increased risk of autoimmune diseases, including both type 1 and type 2 diabetes, rheumatoid arthritis, Crohn’s disease, and multiple sclerosis; infectious diseases; and cardiovascular disease.
For a Quick Guide To the Sunshine Vitamin, Click Here – The Essence of Vitamin D







Pingback: The Essence of Vitamin D
Vitamin D is essential for skeletal health
Vitamin D is necessary for bones
New Roles of Vitamin D are currently being discovered.
you are right, Vitamin D saved my bones
Nice article on role of vitamin D
Here’s My Supplement Facts, I take Calcium, Magnesium, Zinc, and Vitamin D
Pingback: Quora
Hi Adi
I have been reading your articles since beginning and I really appreciate your work. Most attractive thing about this one is valuable information in short and simple manner.
Keep up the good work.
Thanks
This was good to read.
I eat fish for Vitamin D
Thanks for health info
Excellent information on vitamin D – it’s highly appreciable!!
Now I understand Vitamin d fully
This is a top class information.
A lot of thanks for your research on Vitamin D
Lucid yet comprehensive info on Vitamin D
It is true that Vitamin D is also a hormone
It was great to read your article on vitamin D
Really informative article on Vitamin D
Really best on Health and Vitamin D3
You are right Vitamin D is really vital!
Yeah, you rightly explained that Vitamin D is really very vital to health.
very nice info on Vitamin D!!
I think that’s absolutely best stuff.
It is worth sufficient info on vitamins
I like your lucid style